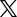-
Stress Fractures more Common for Athletes in Team Sports
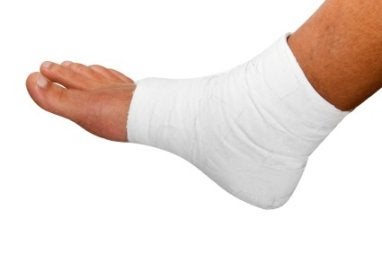 The fifth metatarsal is the long bone that connects to the pinky toe on the outside of the foot. This bone is especially prone to fracture for people involved in any sort of prolonged physical activity, especially team sports. A stress fracture is one of the most common injuries in soccer, but many other athletes also suffer this injury. It is vitally important to never ignore any type of foot pain, on the field or off. Professionally, there is immense pressure to perform, which can lead to dependency on prescription painkillers. But the truth is, we all need our feet, not just star athletes. The best course of action is always to contact a podiatrist and get to the root of the problem.
The fifth metatarsal is the long bone that connects to the pinky toe on the outside of the foot. This bone is especially prone to fracture for people involved in any sort of prolonged physical activity, especially team sports. A stress fracture is one of the most common injuries in soccer, but many other athletes also suffer this injury. It is vitally important to never ignore any type of foot pain, on the field or off. Professionally, there is immense pressure to perform, which can lead to dependency on prescription painkillers. But the truth is, we all need our feet, not just star athletes. The best course of action is always to contact a podiatrist and get to the root of the problem. Activities in which too much pressure is placed on the feet can cause stress fractures. If you have any concerns about your feet contact Dr. Jon M. Sherman of Kentlands Foot & Ankle Center . Our doctor will treat your foot and ankle needs.
Dealing with Stress Fractures of the Foot and Ankle
The Stress Fractures occur on the foot and ankle when muscles in these areas weaken from too much or too little use. Then the feet and ankles lose support when walking or running from the impact of the ground. Since there is no protection the bones receive the full impact of each step. The stress on the feet causes cracks to form in the bones, thus called stress fractures.
What are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Play tennis or basketball
- Gymnastics
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures, and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity that involves in high impact will aggravate pain.
If you have any questions please feel free to contact our office located in Gaithersburg, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Stress Fractures of the Foot and Ankle
-
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step someone takes. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Individuals who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person’s bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
-
Avoiding Plantar Warts
 Working out at the gym can be one important way to maintain good physical health. When exercising in public places, however, there is always an elevated risk of coming into contact with bacteria and viruses that are new to our own personal immune system. Plantar warts are one of the conditions that might crop up when someone is exposed to warm, humid environments. Caused by HPV (human papillomavirus), plantar warts appear as hard, callus like areas on the foot. They can be very painful when even walking around normally. There are various procedures for this condition that range from surgery to laser treatments; consult with your podiatrist to determine the best treatment for you.
Working out at the gym can be one important way to maintain good physical health. When exercising in public places, however, there is always an elevated risk of coming into contact with bacteria and viruses that are new to our own personal immune system. Plantar warts are one of the conditions that might crop up when someone is exposed to warm, humid environments. Caused by HPV (human papillomavirus), plantar warts appear as hard, callus like areas on the foot. They can be very painful when even walking around normally. There are various procedures for this condition that range from surgery to laser treatments; consult with your podiatrist to determine the best treatment for you. Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Jon M. Sherman of Kentlands Foot & Ankle Center . Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Legions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, will help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in Gaithersburg, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about plantar warts.
-
All About Plantar Warts
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.
-
Preventing Athlete’s Foot
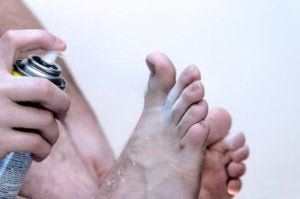 Odor emanates from people’s feet due to sweat or a lack of good hygiene practices. Bacteria can form as a result of either of these two reasons, and it may produce a strong odor . They tend to form around areas that are moist on your feet, and they feed on skin oils and dead cells. When bacteria thrive, they eliminate waste in the form of organic acids, which causes feet to smell. In order to keep your feet bacteria free, you should change your socks daily, keep your toenails clipped and clean, dry feet thoroughly after showering, and swab in between your toes with rubbing alcohol.
Odor emanates from people’s feet due to sweat or a lack of good hygiene practices. Bacteria can form as a result of either of these two reasons, and it may produce a strong odor . They tend to form around areas that are moist on your feet, and they feed on skin oils and dead cells. When bacteria thrive, they eliminate waste in the form of organic acids, which causes feet to smell. In order to keep your feet bacteria free, you should change your socks daily, keep your toenails clipped and clean, dry feet thoroughly after showering, and swab in between your toes with rubbing alcohol. Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact Dr. Jon M. Sherman of Kentlands Foot & Ankle Center . Our doctor can provide the care you need to keep you pain-free and on your feet.
Athlete’s Foot: The Sole Story
Athlete’s foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning and even pain when walking. In the worst cases, athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of athlete’s foot, as well as helping you figure out which treatment options are best for you.
If you have any questions, please feel free to contact our office located in Gaithersburg, MD . We offer the newest diagnostic tools and technologies to treat your foot and ankle needs.
Read more about athlete’s foot.
-
Athlete’s Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
-
What Do Podiatrists Treat?

While most people understand that podiatrists are foot doctors, many people still may not comprehend a podiatrist’s work and the various conditions a podiatrist treats. Various foot problems that many people experience and that a podiatrist can treat include plantar fasciitis, ingrown toenails, bunions, hammertoes, and flat feet.
Among the group who sought podiatric help, 88% reported a quick diagnosis and 76% received treatment that eliminated the problem. A third of the group said that their visits to the podiatrist exposed other health concerns, such as diabetes, circulatory issues, and nerve issues.
“It’s not surprising to see how many people are affected by foot pain, when survey results show that we view our feet as the least important body part in terms of our overall health and wellbeing,” said AMPA President Frank Spinosa. “Our feet are literally and figuratively the furthest things from our minds.”
If you are experiencing pain in the feet or ankles, don’t join the stubborn majority refusing treatment. Feel free to contact Dr. Jon M. Sherman of Kentlands Foot & Ankle Center . Our doctor can provide the care you need to keep you pain-free and on your feet.
What is a Podiatrist?
Someone would seek care of a podiatrist when they have suffered a foot injury or have common foot ailments such as: heal spurs, bunions, arch problems, deformities, ingrown toenails, corns, foot and ankle problems etc.
Podiatric Treatment
A podiatrist will treat the problematic areas of the feet, ankle or lower leg by prescribing the following:
- physical therapy
- drugs
- perform surgery on lower extremity fractures
- orthotic inserts or soles
A common podiatric procedure a podiatrist will use is a scanner or force plate which will allow the podiatrist to know the designs of orthotics. Patients are then told to follow a series of tasks to complete the treatment. The computer will scan the foot a see which areas show weight distribution and pressure points. The podiatrist will read the analysis and then determine which treatment plans are available.
If you have any questions, please feel free to contact our office located in Gaithersburg, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about What is a Podiatrist.
-
What is a Podiatrist
The branch of medicine that is focused on the treatment, diagnosis, and study of disorders of the lower leg, ankle and foot is referred to as podiatry. Because people often spend a great deal of their time on their feet, many problems in this area can occur. A person seeks help from the field of podiatry when they need treatment for heel spurs, bunions, arch problems, deformities, ingrown toenails, corns, foot and ankle problems, infections, and problems with the foot that are related to diabetes and additional diseases.
To treat problems of the foot, ankle or lower leg, a podiatrist may prescribe physical therapy, drugs, perform surgery, or set fractures. Individuals may also be recommended to wear corrective shoe inserts, custom-made shoes, plaster casts and strappings in order to correct deformities.
When trying to gather information on a patient problem, a scanner or force plate may be used in order to design orthotics. During this procedure, patients are told to walk across a plate that is connected to a computer; the computer then takes a scan of the foot and indicates weight distribution and pressure points. The computer readouts will give the podiatrist information to help them determine the correct treatment plans.
Diagnosis is also provided through laboratory tests and x-rays. Through the foot, the first signs of serious problems such as heart disease, diabetes and arthritis can show up. For example, individuals that have diabetes may frequently have problems such as infections and foot ulcers because they experience poor circulation in the foot area. A podiatrist can then have consultations with patients when symptoms arise. Referrals will then be made to specialists that handle the greater health problems.
Some podiatrists have their own independent, private practices or clinics where they have a small staff and administrative personnel. Many podiatrists work within group practices. They usually spend time performing surgery in ambulatory surgical centers or hospitals, or visit patients in nursing homes. Podiatrists typically spend between 30 to 60 hours of week working. Some podiatrists specialize in public health, orthopedics, surgery, or primary care. Other fields include specialties in geriatrics, dermatology, pediatrics, diabetic foot care and sports medicine.
Some podiatrist specialists complete extra training in the area of foot and ankle reconstruction that results from the effects of physical trauma or diabetes. There are also surgeons that perform surgery of a cosmetic nature to correct bunions and hammertoes.
RECENT POSTS
categories
- Uncategorized
- Featured Articles
- Foot Disorders
- Broken Ankle
- Broken Toe
- Fracture
- Foot Health
- Foot Care
- Arthritis
- Foot Pain
- Skin Cancer
- Podiatry Appointment
- Custom Orthotics
- Podiatrist
- Diabetes
- Gout
- Heart Health
- National Nutrition Month
- National Foot Health Awareness Month
- Foot Safety
- Foot and Ankle Injuries
- Falls Prevention
- Chronic Heel Pain
- Shoes
- Laser Therapy
- Quoted
- Physical Therapy
- KeryFlex
- Sweat
- Summer Foot Care
- Sports Injury
- ESWT
- Fungal Toenails
- Bunion
- Plantar Fasciitis
- PinPointe Laser
- Heel Pain
- walking